Labrum & Biceps Repair
Labral Repair
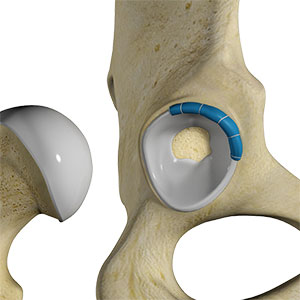
Anatomy of the Shoulder Labrum
The shoulder joint is a ball and socket joint. A 'ball' at the top of the upper arm bone (the humerus) fits neatly into a 'socket', called the glenoid, which is part of the shoulder blade (scapula). The labrum is a ring of fibrous cartilage surrounding the glenoid, which helps in stabilizing the shoulder joint. The biceps tendon is attached inside the shoulder joint at the superior labrum of the joint. The biceps tendon is a long cord-like structure which attaches the biceps muscle to the shoulder and helps to stabilize the joint.
Shoulder Labral Tears
Traumatic injury to the shoulder or overuse of the shoulder by excessive throwing or weightlifting can cause a labral tear. In addition, the ageing process may weaken the labrum, leading to injury secondary to wear and tear.
Symptoms of Shoulder Labral Tears
A shoulder labral tear injury can cause symptoms such as pain, a catching or locking sensation, decreased range of motion and joint instability.
Types of Shoulder Labral Tears
The most common types of labral tears include:
- SLAP tear: The term SLAP (superior–labrum anterior-posterior) refers to an injury of the superior labrum of the shoulder, at the attachment of the biceps tendon.
- Bankart tear: A Bankart tear is an injury to the labrum that leads to recurrent dislocations and arthritis of the shoulder.
- Posterior labrum tear: This type of labrum tear is rare, but may be caused by repeated internal impingement, where the extreme extension and external rotation of the shoulder joint causes pinching of the bulged part of the arm bone against the lining of the shoulder joint cavity.
Diagnosis of Shoulder Labral Tears
Your doctor may suspect a labral tear based on your symptoms and medical history. The doctor will inquire about your pain and history of injury. Several physical tests will be performed by your doctor to evaluate the range of motion and stability of your shoulder. X-rays may be used to rule out other conditions. Your doctor may also order a computed tomography (CT) scan or magnetic resonance imaging (MRI) scan, with a contrast medium, to determine the presence of tears. Diagnosis of a labral tear can also be confirmed through shoulder arthroscopy.
Conservative Treatment of Shoulder Labral Tears
Your doctor may start with conservative approaches such as prescribing anti-inflammatory medications and advise rest to relieve symptoms. Rehabilitation exercises may be recommended to strengthen the rotator cuff muscles. If the symptoms do not resolve with these conservative measures, your doctor may recommend arthroscopic surgery.
Surgical Treatment of Shoulder Labral Tears
During arthroscopic surgery for SLAP tears, your surgeon examines the labrum and the biceps tendon. If the damage is confined to the labrum without involving the tendon, then the torn flap of the labrum will be removed. In cases where the tendon is also involved or if there is detachment of the tendon, absorbable wires or sutures will be used to repair and reattach the tendon.
Bankart lesion is repaired by a Bankart operation. In this procedure, the Bankart tear is repaired by reattaching the labrum and the capsule to the anterior margin of the glenoid cavity. Your surgeon makes a few small incisions around the joint. Through one incision, an arthroscope is inserted into the shoulder to visualize the inside of the shoulder joint. Other surgical instruments are inserted through the other incisions to re-attach the labrum to the glenoid with the help of sutures or anchoring devices. The arthroscope and surgical instruments are removed and the incisions are closed.
Postoperative Care for Shoulder Labrum Reconstruction
Following the surgery, your shoulder is immobilized with a sling for a few days. To control pain and swelling, your physical therapist may use ice, electrical stimulation, massage therapy, and other hands-on treatments. Passive range of motion exercises are also initiated in the post-operative phase. Active range of motion exercises is started about 6 weeks after the repair, to regain your shoulder movement. Athletes can return to sports in about three months.
Risks and Complications of Shoulder Labrum Reconstruction
The risks associated with a labral reconstruction include:
- Nerve injury
- Wound infection
- Tear of the repair
- Shoulder stiffness
- Recurrence of instability
- Poor positioning of anchor suture
- Failure of the repair
Biceps Repair
What is a Bicep Tendon Tear?
The biceps muscle, located in the front of the upper arm allows you to bend the elbow and rotate the arm. Biceps tendons attach the biceps muscle to the bones in the shoulder and in the elbow.
Biceps tear can be complete or partial. Partial biceps tendon tears will not completely break the tendon. Complete tendon tears will break the tendon into two parts.
Biceps tendon tears at the elbow: Although two tendons attach the biceps muscle to the bone at the shoulder, only one tendon attaches it to the elbow. This is known as the distal biceps tendon. Tears of the distal biceps tendon are usually complete and the muscle is separated from the bone. Tears of the distal biceps tendon most often result from a sudden injury or lifting a heavy object.
Causes of Bicep Tendon Tears
Biceps tendon tear can be caused by injury such as falling with your arm outstretched or during the act of lifting heavy objects. In case of overuse, a tendon may fray and eventually tear. Other shoulder problems such as tendonitis, shoulder impingement, and rotator cuff injuries are more likely to weaken or tear the biceps tendon. Additional risk factors such as advancing age, heavy overhead activities, repetitive overhead sports, smoking, and use of corticosteroids can also result in a tendon tear.
Symptoms of Bicep Tendon Tears
The most common symptom is a sudden, severe pain in the upper arm or at the elbow, depending on where the tendon is injured. At times, you may hear a “pop”. Other symptoms include swelling, visible bruising, weakness in the shoulder or elbow, and trouble turning your palm up or palm down. A bulge referred to as a “Popeye Muscle,” may also appear in your arm, because the tendon is no longer holding the muscle in place properly.
Diagnosis of Bicep Tendon Tears
Biceps tendon tear is usually diagnosed based on your symptoms, medical history, and a physical examination. During the physical examination, your doctor will look for a gap in the front of the elbow. Your doctor will diagnose a partial tear by asking you to bend your arm and tighten the biceps muscle. You may have pain if there is a partial tear. X-rays may be taken to rule out other conditions causing shoulder and elbow pain. Using an MRI scan, your doctor can know whether the tear is partial or complete.
Treatment Options for Bicep Tendon Tears
Non-surgical Treatment Options for Bicep Tendon Tears
Conservative treatment for a proximal biceps tendon tear includes:
- ice application
- limiting activity
- non-steroidal anti-inflammatory medications to reduce the pain and keep down the swelling
- flexibility and strengthening exercises to restore the mobility and strengthen the surrounding muscles
Surgery for Bicep Tendon Tears
Surgery to reattach the torn tendon back to the bone is rarely needed. However, for patients with partial tears who continue to experience symptoms after non-surgical treatments or who want all their arm strength back, such as athletes or manual laborers, surgery may be the best option.
Your surgeon may opt for several surgical procedures for distal bicep tendon tear where the distal biceps tendon is reattached to the forearm bone. Some doctors would instead use two incisions, while some use only 1 incision. Both procedures carry certain advantages and disadvantages. During the procedure, the tendon is attached with stitches through holes drilled inside the bone or small metal implants may be used to attach the tendon to the bone.
Post-surgical Care for Bicep Tendon Tears
Following surgical repair, you will need to do flexibility and strengthening exercises to improve the range of motion in your shoulder.
Risks and Complications of Bicep Tendon Tears
Complications are rare and may include numbness and weakness in the forearm, formation of new bone, limited movement, and tearing may recur.
